Almost every week at our Legazpi Village clinic, a patient walks in with a story that goes something like this: "Doc, masakit na po yung likod ko for almost a year now. I've been taking mefenamic, I've tried massage, I've been resting — bakit hindi pa rin nawawala?" The short answer is because chronic pain is not the same creature as acute pain. The longer answer — which we are about to walk through — is both reassuring and deeply useful, because it points to things that actually work.
Acute pain vs chronic pain: two different conversations
When you step on a nail or twist an ankle coming off a jeepney, your nervous system does something brilliant. Pain receptors in the tissue fire, signals race up the spinal cord to the brain, and within milliseconds you feel sharp, localized pain. That is acute pain, and it is protective. You yank your foot away; you limp off the bad ankle; tissue heals in six to twelve weeks; the pain switches off. Clean loop.
Chronic pain is defined as pain that lasts more than three months — long past the point where most tissues have healed. Under the microscope we often find the original injury is gone, yet the pain persists. Why? Because the nervous system itself has changed. Your spinal cord and brain have become better and better at transmitting pain signals, a process called central sensitization. It is a real, measurable phenomenon — and it is the reason rest, mefenamic, and good intentions often stop working past a certain point.
Neuroplasticity: the good news hidden in the bad news
Here is the part most patients have never heard. The same nervous system that learned how to amplify pain can also learn to quiet it. Neuroplasticity — your brain's ability to rewire itself throughout life — is a two-way street. Through specific movements, graded exposure, and (yes) a different way of talking to your own body, we can train the pain gates to close again. This is not positive thinking. It is a clinical process with decades of research behind it.
The gate control theory, first proposed in the 1960s and updated many times since, describes how the spinal cord has something like a dimmer switch for pain. When you rub a bumped elbow and it feels better — that is a gate closing in real time. Chronic pain changes the default position of that dimmer. Our job, and yours, is to gradually turn it back down.
Why rest often makes chronic pain worse
This is the hardest message for Filipino patients to hear, because we are raised on "magpahinga ka muna." For acute pain in the first few days, yes — protect the tissue. But after about two weeks of rest, chronic pain actually worsens. Here is what happens:
- Muscles deconditioned — in ten days of bed rest you can lose 10 to 15 percent of leg strength. Weaker muscles mean more strain on joints, which means more pain signals.
- Joints stiffen — cartilage depends on movement to get its nutrition. Immobility literally starves your joints.
- The brain re-maps the painful area — if you avoid bending, the circuits that handle bending become more sensitive, not less. Your brain treats the movement as threatening even when nothing is wrong.
- Mood and sleep collapse — which are themselves major pain amplifiers.
We see this cycle in almost every patient who has been told "avoid doing X until it stops hurting" — they come in after twelve months having avoided X, and the pain has only grown.
Tip from our team
The word "hurt" and the word "harm" are not the same thing. A movement can hurt (fire pain signals) without harming (damaging tissue). Relearning this distinction is often the first turning point in chronic pain recovery — and it is something a good physical therapist will walk you through, movement by movement.
Medication vs movement: not an either-or
We are not anti-medication. For acute flares, short-term NSAIDs can be useful. For some chronic pain conditions — neuropathic pain, fibromyalgia — certain medications prescribed by your physician genuinely help. The problem is when patients end up on long-term painkillers as the only strategy, sometimes for years, while the underlying drivers (deconditioning, postural habits, poor sleep, fear-avoidance of movement) are never addressed. The pain always comes back, usually worse.
A well-structured active approach works alongside your doctor, not against them. We routinely coordinate with orthopedics at Makati Med, St. Luke's and Asian Hospital — sending progress notes, clarifying restrictions, stepping therapy up or down as your medical team adjusts your plan.
What actually helps: the evidence-based stack
1. Graded exposure to movement
The single most effective intervention in chronic musculoskeletal pain is a carefully dosed reintroduction of the movements your nervous system has started to fear. We start below your pain threshold and build up week by week. For a patient with chronic lower back pain, this might look very similar to the progression we describe in our lower back pain guide for Manila commuters.
2. Pain education itself
Understanding why your pain persists — the same information you are reading now — has been shown in multiple trials to reduce pain intensity on its own. It is not mind over matter. It is your brain downgrading a signal from "emergency" to "manageable."
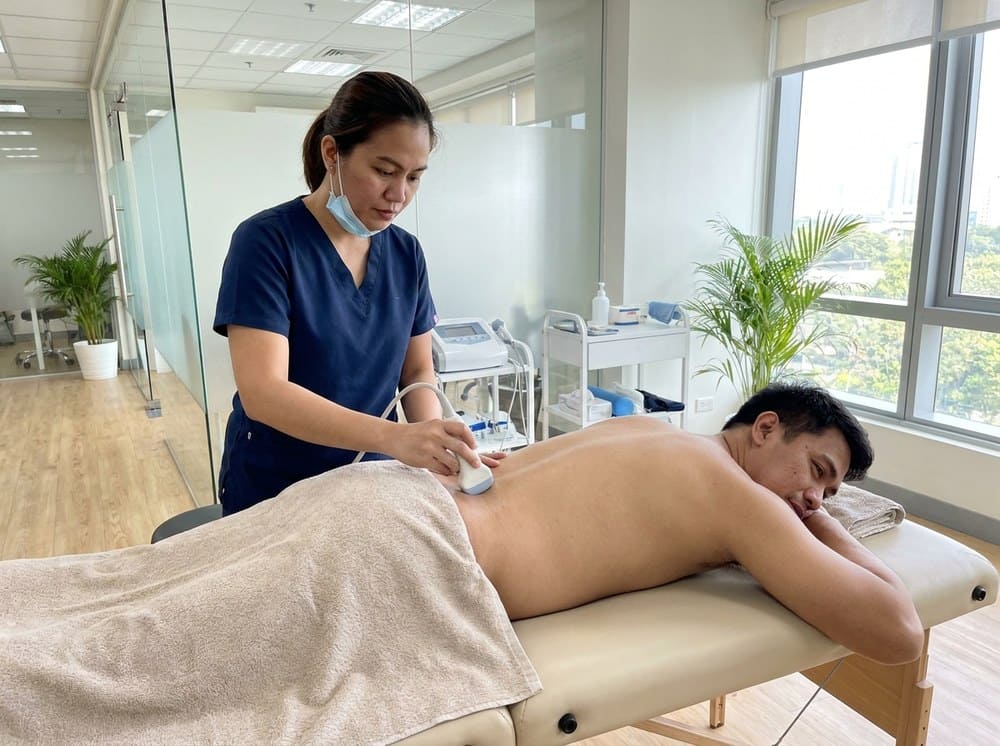
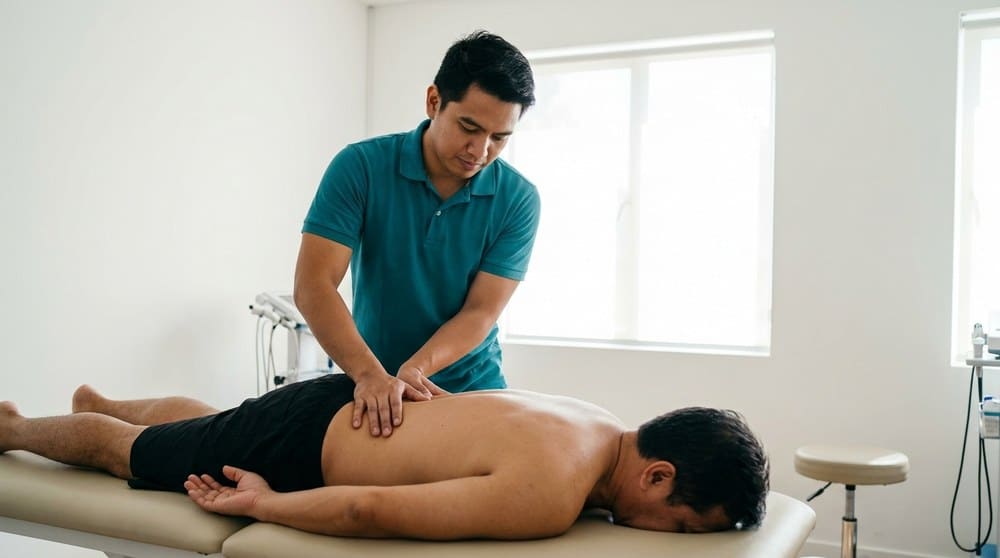
3. Manual therapy as a window, not a solution
Hands-on techniques, dry needling, and soft-tissue work can reduce pain enough to let you start moving again. We use them as doorways into active rehab — not as weekly maintenance you depend on forever.
4. Sleep, stress, and the nervous system
A night of poor sleep raises pain sensitivity by up to 30 percent the next day. Chronic work stress has a similar effect. We are not therapists, but we are trained to spot when these factors are keeping you stuck, and we will gently flag it.
5. Addressing the specific body region properly
If your chronic pain is centered on one joint or area, it still needs condition-specific care. Our back pain relief and shoulder therapy programs, for example, combine all of the above with targeted hands-on techniques for each region.
The Filipino context: "tiis-tiis lang" is a trap
Filipino culture has a deep admiration for stoicism — enduring pain quietly, not wanting to be a burden, prioritizing family over yourself. Those are beautiful values, but they are catastrophic for chronic pain. The patients who wait the longest to seek care — two years, five years, a decade — are the ones whose nervous systems have had the most time to remodel around pain. They are harder (not impossible) to treat.
Rule of thumb: if pain has been with you for more than 6 weeks and is not clearly improving, it is time to see someone. Not because something is necessarily "wrong," but because the earlier we interrupt the sensitization process, the easier and faster recovery is.
What a chronic pain assessment actually looks like at our clinic
When you come in for a first visit, we spend 45 to 60 minutes on assessment — far longer than you get at most clinics. We ask about the story of your pain, your work, your commute, your sleep. We test movement, strength, and which positions aggravate or ease symptoms. We explain — in Tagalog or English, whichever you prefer — what we think is driving things. Then we build a plan with you, not for you.
Most chronic pain patients see meaningful improvement within 6 to 12 sessions. Some people need fewer, some need more. Whatever we do, we teach you to do it independently, because the goal is not to keep you dependent on us. The goal is to get you back to jogging BGC, carrying apo, gardening, typing for work, whatever you value.
A final, hopeful note
Chronic pain is real. It is not "in your head" in the dismissive sense — it is in your nervous system, which is a very different claim. And exactly because it lives in a system that is built to adapt, change is always possible, even after years. Some of the most moving recoveries we have been part of were patients in their 60s and 70s who had given up on ever feeling normal again.
If that sounds like you, or like a tita or lolo in your life, we are glad to talk. A first assessment is free, and nothing is lost by understanding your situation better.
Thinking it might be time?
Book a free 20-minute assessment with one of our licensed DPTs. HMO billing supported, and we will give you an honest read on whether physical therapy is the right next step for you.
Book Assessment Call +63 917 428 6391 By Dr. Marianne Aquino, DPT
By Dr. Marianne Aquino, DPT