Pain kills quality of life. It stops you from carrying your apo, from finishing a 5K, from sleeping through the night, from enjoying a family trip to Baguio. And yet, the treatment menu most Filipinos are offered is still narrow: mefenamic, biogesic, maybe a tramadol prescription, and if it keeps hurting, eventually an MRI and a surgical consult. That is a real menu, but it is not the whole menu. Below are seven additional, well-researched approaches we use at our Makati clinic — with honest notes on what each one is really good for.
1. Physical therapy (the umbrella)
Physical therapy is the clinical discipline, not a single technique. A licensed PT in the Philippines (look for PTRP or DPT credentials verified on the PRC license lookup) combines assessment, hands-on care, exercise therapy, education, and often several of the tools below into one personalized plan. The strongest evidence for PT as a first-line option is in:
- Most musculoskeletal pain — back, neck, shoulder, knee, hip.
- Post-surgical recovery — from ACL to joint replacement to spine.
- Chronic pain, especially when it has become complex over time (see our article on chronic pain).
Think of a PT as the coordinator of your care: someone who can do some techniques themselves, and who knows when to refer on.
2. Manual therapy
Manual therapy is a broad category of hands-on techniques: joint mobilization, soft tissue release, myofascial work, trigger point therapy. It is one of the fastest ways to temporarily reduce pain and increase range of motion, which creates the window in which the more lasting work (exercise, behavioral change) can happen.
Good for: acute muscle spasm, joint stiffness, post-surgical scar tissue, trigger-point-driven headaches.
Not a cure for: structural joint damage or serious radiculopathy — manual therapy can ease those symptoms but will not reverse the underlying condition.
Honest note: a weekly massage is not manual therapy. Manual therapy is targeted, based on assessment, and progressively dosed across a plan of care. If you have been getting the same treatment every week for six months with no progression, that is not therapy — that is maintenance.
3. Shockwave therapy
Extracorporeal shockwave therapy (ESWT) uses focused acoustic pressure waves to stimulate healing in stubborn soft-tissue conditions. It does not involve electrical shocks — the name is a translation quirk. Strongest evidence is for:
- Plantar fasciitis (chronic heel pain).
- Calcific tendinopathy of the shoulder.
- Achilles tendinopathy.
- Tennis/golfer's elbow (lateral/medial epicondylitis).
- Some cases of patellar tendinopathy.
Typical protocol: 3 to 6 weekly sessions. Results are often felt within the first two but may continue building for up to 12 weeks after the last session.
Honest note: it is not a magic wand. It works best combined with structured rehab — not as a standalone. If a clinic offers shockwave alone with no exercise program, that is a red flag.
Tip from our team
When evaluating any pain management option, ask two questions: "What is the evidence this works for my specific condition?" and "What am I going to do to consolidate the gains?" Anything that does not address both is a short-term fix at best.
4. Dry needling
Dry needling uses thin acupuncture-style needles (hence the name — they are "dry" because nothing is injected) to target myofascial trigger points — the small, hyper-irritable knots you can often feel as "balls" in tight muscles. Done correctly, it produces a brief local twitch response and a subsequent release of the taut band.
Good for: trigger-point-driven neck, shoulder, and back pain; stubborn muscular knots that have not responded to manual therapy alone; some forms of tension headache.
Important: dry needling is different from acupuncture. Same tools, different theory and targeting. In the Philippines, it should be performed only by a trained and licensed physical therapist, physician, or other qualified clinician.
Honest note: it is uncomfortable for the first minute. Most patients say it is worth it. If you have a strong needle phobia, we start with non-needle options.
5. Exercise therapy (the most boring one that works the best)
This is the option that looks least glamorous on a marketing page but consistently comes out on top in clinical trials. A structured, progressive exercise program — addressing strength, mobility, motor control, and cardiovascular fitness — is the single most well-supported treatment for chronic low back pain, knee osteoarthritis, chronic neck pain, and many types of tendinopathy.
Key word: structured. Random YouTube stretches are not exercise therapy. A program built for your specific condition, assessed and progressed by a clinician, is. It is also the option that has the best chance of preventing recurrence — which is why every package we offer at the clinic ends with a home program, not just "come back next week."
If you want to see how this is integrated with condition-specific care, have a look at our knee and arthritis program or our sports injury recovery program.
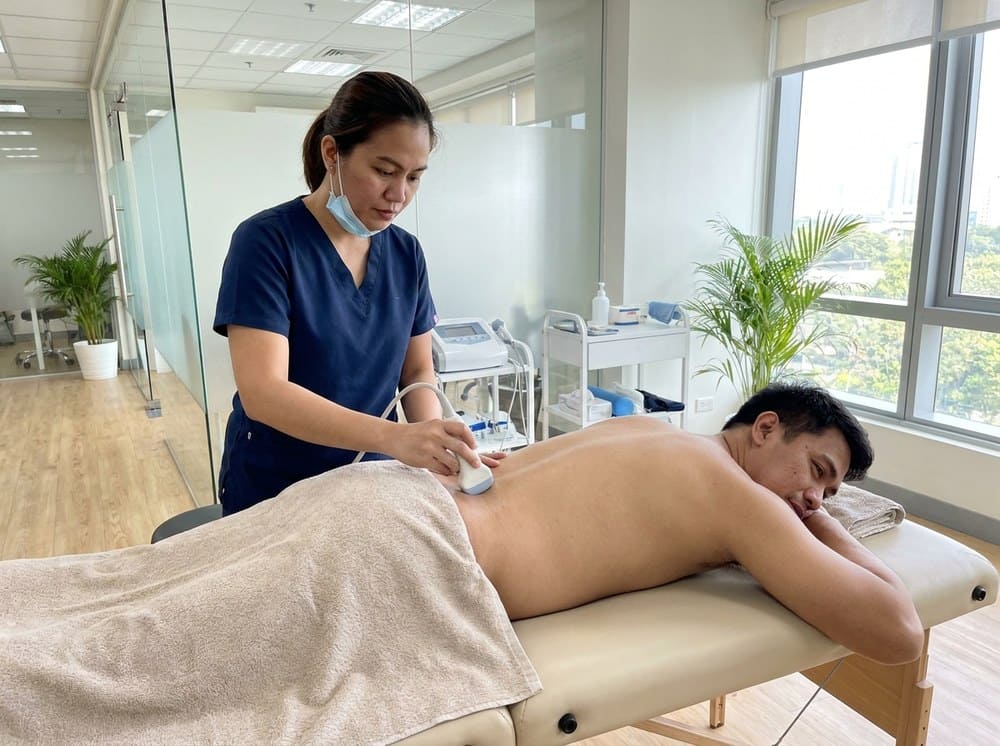
6. Heat, ice, and other modalities
These are the oldest tools in the box, and they still have their place. Heat helps muscular tension and chronic stiffness; ice helps acute inflammation and swelling within the first 48 hours. Ultrasound, TENS, and interferential current — collectively called electrotherapy — can be mildly helpful for some conditions, but the evidence is modest. They are supportive tools, not main-event treatments.
For when to use which, see our dedicated heat vs ice therapy article.
7. Mindfulness-based pain management
This one often gets dismissed as "soft," which is a shame because it has some of the strongest evidence for chronic pain in the entire literature. Mindfulness-based stress reduction (MBSR) and acceptance and commitment therapy (ACT) techniques — essentially training your attention to relate differently to pain signals — have been shown to:
- Reduce chronic pain intensity.
- Lower the disability associated with pain.
- Improve sleep and mood — both of which amplify pain when disturbed.
- Reduce long-term medication use.
We are physiotherapists, not psychologists — but we do incorporate simple mindfulness and breathing practices into many of our chronic pain plans, and we refer to psychologists we trust when the need goes beyond what we can offer.
Pro tip: Filipino culture's strong religious and community ties actually make mindfulness-based techniques easier to adopt than in many other contexts — the same skills you bring to prayer translate well. Do not dismiss this option just because it sounds modern.
How to pick the right stack for your specific pain
The real work of pain management is figuring out the right combination for your specific situation. A 25-year-old with a fresh ACL rehab need is a very different case from a 58-year-old with 10 years of lower back pain and high stress. What looks the same on paper — "pain management" — is wildly different in practice.
A good first assessment should cover:
- Your goals. Not just "less pain" — what do you want to do again?
- The condition's history. When did it start, what makes it worse, what makes it better?
- What you have already tried. So we do not repeat what did not work.
- Your lifestyle. Your job, commute, family situation, sleep. All affect what will work for you.
- Your preferences. Afraid of needles? We adapt. Love exercise? We lean harder on that.
What about surgery and meds — when do they come in?
Surgery is the right answer for some conditions — severe end-stage osteoarthritis, major rotator cuff tears with weakness, significant nerve compression, fractures. A good physiotherapist will not hide this from you. If we see signs your case needs orthopedic evaluation, we will refer you to a surgeon at Makati Med, St. Luke's, or Asian Hospital — we coordinate with specialists there regularly.
Medication also has its place. Short-term NSAIDs after an acute injury, disease-modifying drugs for inflammatory arthritis, neuropathic agents for specific nerve pain syndromes. What we try to avoid is patients sitting on long-term mefenamic for months while nothing else is being done. If that describes you, let us talk about a better plan.
A final word on choosing a provider
The single most important factor in how well pain management works is who you see. Look for:
- A PRC-licensed physical therapist (PTRP or DPT). Check the PRC website — it is free to verify.
- Clinical experience in your specific type of complaint.
- A clear assessment before any treatment starts — no generic "packages."
- Home exercises as part of the plan from the beginning.
- Honest communication about expected timelines and when to escalate.
Not sure which options make sense for you?
Book a free 20-minute assessment. We will walk through what we think would actually move the needle for your specific case, and we will tell you honestly if we are not the right fit.
Book Assessment Call +63 917 428 6391 By Dr. Marianne Aquino, DPT
By Dr. Marianne Aquino, DPT